Cardiology Billing: Heart-Healthy Solutions Unveiled March 21, 2024
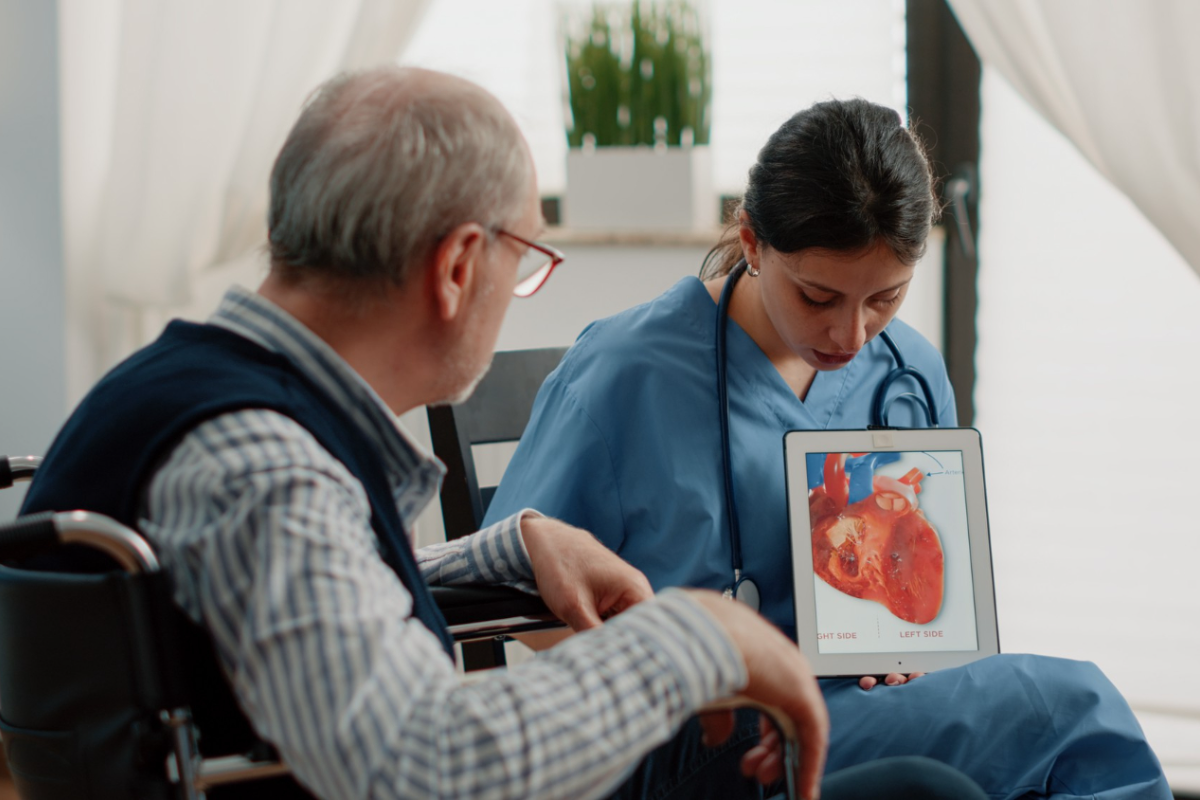
Explore cardiology billing solutions designed to optimize practice performance. Take your cardiology practice to the next level with efficient billing solutions.

Explore cardiology billing solutions designed to optimize practice performance. Take your cardiology practice to the next level with efficient billing solutions.

Learn how advancements in artificial intelligence (AI) are streamlining billing processes, increasing accuracy, and improving revenue cycle management in healthcare.

Unlock the secrets of efficient medical billing in 2024 with our guide. This blog covers the latest industry regulations to cutting-edge techniques to optimize revenue.

Explore the changing dynamics of denial management within value-based care models, uncovering key insights to navigate this shifting terrain effectively.
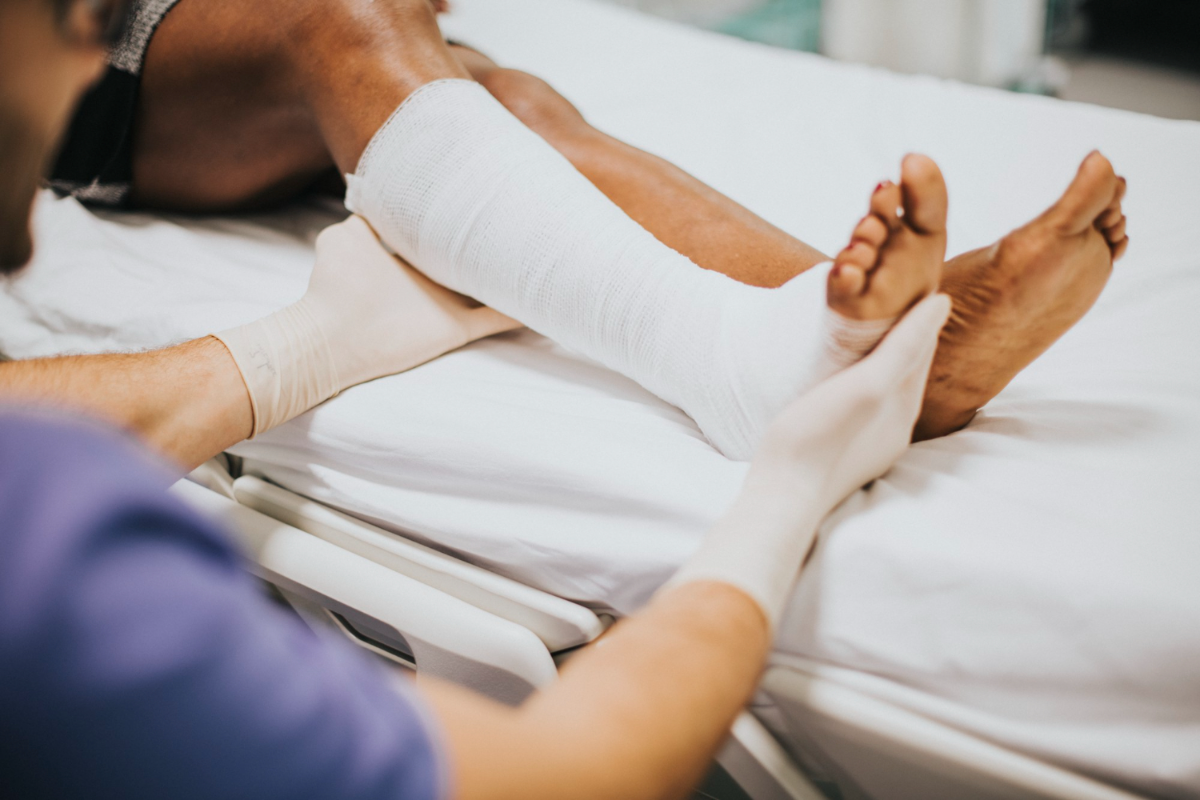
Optimal efficiency and accuracy are being prioritized by orthopedic practices in 2024. Discover how streamlined approaches enhance revenue generation and practice management, driving success in the dynamic healthcare landscape.

Learn vital strategies for preventing physician burnout. Prioritize well-being, build resilience, and create a fulfilling medical career with actionable insights.

Dive into the future of medical coding with our 2024 ICD-10-CM Code Guideline Resources.

Unlock the power of precision in medical billing with our 2024 CPT Code Guides Resources. Stay ahead of industry changes, streamline coding processes, and ensure accurate reimbursement.

In the dynamic landscape of healthcare administration, OBGYN billing and compliance stand at the forefront, demanding a delicate balance between financial efficiency and ethical practices.

Discover emerging trends and innovations in physician credentialing. Gain valuable insight into how medical credentialing is evolving in the healthcare industry.